Lung cancer, what to do?
update septembre 2018
notes by dr. Claudio Italiano

 Meanwhile, the first thing to do is to know what to look for, because the doctor
does not always know it! In fact, before making a diagnosis, it is necessary to
have carried out the proper investigations and to have carried out the
instrumental assessments of the case. If a patient always has cough or chronic
bronchitis, a neoplastic lesion should be suspected that underlies the pathology
I am treating.
Meanwhile, the first thing to do is to know what to look for, because the doctor
does not always know it! In fact, before making a diagnosis, it is necessary to
have carried out the proper investigations and to have carried out the
instrumental assessments of the case. If a patient always has cough or chronic
bronchitis, a neoplastic lesion should be suspected that underlies the pathology
I am treating.
 Often the signs are strange: a patient had lost weight and could no longer feed
as he should. Initially aside from an insistent cough, the patient loses weight
and does not feed, has disgust for the foods he previously thought to be appetizing,
presents dyspnea, chest pain, blood-stained or frankly blood-stained sputum,
bone pain especially if metastases are present , clubbing, serotine fevers,
fever that heals by antibiotic treatment but then resumes,
asthenia. Other times it shows signs of
relevance of the mediastinal syndrome.
Often the signs are strange: a patient had lost weight and could no longer feed
as he should. Initially aside from an insistent cough, the patient loses weight
and does not feed, has disgust for the foods he previously thought to be appetizing,
presents dyspnea, chest pain, blood-stained or frankly blood-stained sputum,
bone pain especially if metastases are present , clubbing, serotine fevers,
fever that heals by antibiotic treatment but then resumes,
asthenia. Other times it shows signs of
relevance of the mediastinal syndrome.
The symptoms are:
Cough 75% of cases - Weight loss 68% -Dispnea 58-60% - Chest pain 45-49% -
Hemoptysis 29-35% - Bone pain 25% - clubbing 20% - Fever 15-20% - Asthenia 10%
- syndrome of the vena cava sup: 4%
Lung cancer is sneaky and insidious, especially the scaly one (see Lung cancer).
After performing a standard chest radiography survey (see Chest X-ray Standard
Chest X-ray Examples), if I have suspicions you should always ask for a chest CT
scan also without contrast and complete the investigation with biopsies targeted
to the identified lesions. as such or suspicious.
In fact, the pre-therapeutic moment uses cytology, histology, histochemistry,
immunocytochemistry and electron microscopy. But even the cytological finding
can give false negatives; if instead there are suspicions, it is good to
indicate the histological type or simply if we are facing the microcitome. If
the cells are dysplastic, or atypical only for inflammatory, regenerative
phenomena or if, rather, cells are really neoplastic.
Symptoms and signs at the time of the visit
General: weight loss> 5 kg Musculoskeletal: focal skeletal pain
Neurological: headache, syncope, convulsions, weakness
Signs for the objective examination: Peripheral lymphadenomegaly (> 1 cm)
Hoarseness, VCS syndrome
Bone pain in the pressure
Hepatomegaly (> 13 cm)
Palpable masses
Laboratory tests: Hematocrit <40% (man) or <35% (women)
Alkaline phosphatase, ALT and AST increased
Paraneoplastic syndromes associated with pulmonary carcinoma
We speak about a systemic syndrome when the same pathological substrate is able to
provoke and support clinical pictures that affect all the organism. The most
frequent systemic syndromes are cachexia and fever. Both these frameworks are
mainly due to the exuberant production of TNF-α (also called cachesin); in
particular, the cytokines IL-1 and IL-6, produced by the inflammatory cells are
also involved in the genesis of fever, as they are able to raise the
hypothalamic thermal set-point and trigger the mechanisms that lead to the
increase in temperature.
Another manifestation, always cytokino-correlated and
often detectable systemic, is normochromic normocytic anemia that testifies to
the presence of a chronic disorder. Migrant thrombophlebitis, in a thrombophilic
context. In other cases, the tumor, e.g. the microcitome, secretes hormonal
substances.
- Endocrine: - Cushing syndrome (ACTH) - Hypercalcemia (PTH, PTH-RP, PGE2): SCC
- Hypocalcaemia (calcitonin) - Hypophosphatemia - Inappropriate secretion of ADH
(SCLC) - Gynecomastia (gonadotropins) - Somatostatinoma syndrome - Carcinoid
syndrome -Hypoglycemia
- Neuromuscular: - Limbic encephalitis - Subacute cerebellar degeneration -
Spino-cerebellar degeneration - Transverse myelitis - Peripheral neuropathy -
Lambert-Eaton syndrome - Polymyositis
-Deleletal / articular: -Digital Hippocratism - Hypertrophic pulmonary
osteoarthropathy 4) Dermal: - Lymphatic hypertrichosis - Erythema shot -
Seborrheic keratosis - Acanthosis nigricans
- Cardiovascular / Hematology: - Migratory thrombophlebitis (Trousseau syndrome).
- CID -Anemia, leukemoid reaction, eosinophilia, platelets - non-bacterial (marantic)
Endocarditis -
- Renal: - Nephrotic syndrome (glomerulopathy with minimal lesions)
- Systemic: - Fever, anorexia, cachexiaEpidemiologia
Symptoms and signs at the time of the visit
General: weight loss> 5 kg Musculoskeletal: focal skeletal pain
Neurological: headache, syncope, convulsions, weakness
Signs for the objective examination: Peripheral lymphadenomegaly (> 1 cm)
Hoarseness, VCS syndrome
Bone pain in the pressure
Hepatomegaly (> 13 cm)
Palpable masses
Laboratory tests: Hematocrit <40% (man) or <35% (women)
Alkaline phosphatase, ALT and AST increased
 • Currently lung cancer is the most frequent malignant neoplasm and the main
(17% of all cases) cause death from neoplasm in the world both in males (24% of
all cases) and in females (10% of all cases ) with over 3,000 deaths a day
worldwide.
• Currently lung cancer is the most frequent malignant neoplasm and the main
(17% of all cases) cause death from neoplasm in the world both in males (24% of
all cases) and in females (10% of all cases ) with over 3,000 deaths a day
worldwide.
• The incidence of lung cancer is continuously increasing. Lung cancer was
fairly rare in 1950, and the lung cancer mortality rate rose 225% in males and
330% in women in the 1950s and 1980s.
In Italy there are currently about 41,000 new cases of lung cancer each year
with about 33,700 (25,150 males and 8,550 females) died each year from lung
cancer.
• In Italy at present the risk of having a lung cancer diagnosis in the course
of life (between 0 and 74 years) is equal to 1 case for every 15 men and 1 case
for every 71 women.
Practical classification of pulmonary neoplasms
• Pulmonary neoplasms can be classified into primitives and secondary ones.
• Primary pulmonary neoplasms may be benign or malignant, but about 90-95% of
them are carcinomas, about 5% are bronchial carcinoids and 2-5% are mesenchymal
and other origin neoplasms.
Secondary pulmonary neoplasms are always malignant, very frequent (the lung is
one of the most frequent metastatic sites of extrathoracic neoplasms). 20-50% of
all patients with extrapulmonary solid tumors at autopsy have lung metastases
and in 15-25% of cases the lung is the only metastatic site. The neoplasms with
greater propensity to pulmonary metastases are malignant melanoma, some sarcomas
(Ewing, osteosarcoma), breast, prostatic, renal, uterine and thyroid carcinoma,
testicle germ cell neoplasms and uterine choriocarcinoma.
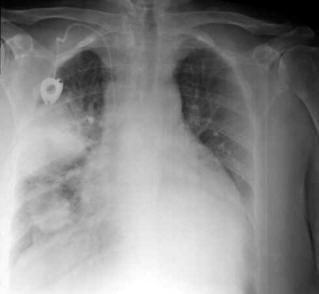
chest X-ray: Carcinoma of the lung, in the
middle and lower field of the right lung, two thickening lesions are
appreciated, with shaded margins |
Cytology
The cytological investigation must be carried out on:
Sputum, usually on 3-5 samples, obtained after heated aerosol, always fresh and
in a short time, fixing the cells in alcohol.
Bronchoalveolar lavage.
The material can be swiped on a slide and fixed with spray (citofix), with
coloring and immediate reading, or collected in a container and fixed with
formalin or alcohol.
Broncho-alveolar washing fluid (BAL)
The examination is performed in patients. symptomatic. The material is collected
in a container and fixed in formalin in equal quantities.
Bronchial brushing.
It is performed in symptomatic patients. The material is swiped on a slide and
fixed with a citofix.
Fine needle aspirator (FNAB), also eco or guided TC. It is executed in pcs.
symptomatic. The material is swiped on a slide and fixed with a citofix.
Pleural fluid
The exam is performed in pcs. symptomatic. The liquid is collected in a
container and fixed in formalin in equal quantities.
Lung tumors are divided into:
A) NonSmall Cell Lung Cancer (NSCLC = non-small cell lung cancer): large cell,
adenocarcinoma and squamous cell carcinoma
B) and Small Cell Lung Cancer (SCLC = small cell lung cancer or microcytoma)
Biotic withdrawals
They can come from:
1. Bronchial biopsy (it is the most used method, for central neoplasms);
2. Transbronchial pulmonary biopsy (cases with endoscopy and negative cytology);
3. Transparietal metabolic biopsy of CT guided (peripheral neoplasms with
negative endoscopy);
4. Pleural biopsy under endoscopic control (peripheral neoplasms or central
neoplasms for the evaluation of the spread of the neoplasia);
5. Thoracotomy pulmonary biopsy (for intraoperative extemporaneous examination);
6. Mediastinal biopsy (during mediastinoscopy or by mediastinotomy);
7. Biopsy on presumed distant metastases (osteomidullary biopsy, liver disease
etc.).
Biopsies are used in the clinical phase of the disease and allow the assessment
of the existence of a neoplasm and its typing. The examination can be performed
by paraffin embedding (histological examination by inclusion) or by cryostat
freezing (extemporaneous intraoperative histological examination). The tissue
sampling should be as wide as possible, in an area free from phlogistic-necrotic
phenomena, preferably in multiple fragments to prevent the material from being
insufficient, fixed in formalin 10%, in adequate quantities (1:20 ratio);
fragments for extemporary histological examination must be delivered fresh.
Histochemistry
Histochemistry is used in the typing of lung carcinoma. P.A.S. reaction after
digestion with diastase, blue Alcian and mucicarminium staining demonstrate the
presence of mucins (adenocarcinoma, adenosquamous carcinoma).
Immunocytochemistry is useful in the diagnosis and in the typing of tumors (cytokeratins,
carcinoembryonic antigen, neurofilaments, etc.). Neuron-specific enolase (NSE),
chromogranin, synaptophysin, CD57 are used to demonstrate the neuroendocrine
phenotype of small cell carcinoma (microcitoma) or neuroendocrine
differentiation areas. In the differentiation in bioptic fragments of limited
size between epithelial pleural mesothelioma and adenocarcinoma antibodies
(AMAD-2) are used which recognize antigens associated with mesothelioma and are
usually not expressed by pulmonary adenocarcinomas or metastatic carcinomas of
the pleura.
Staging
Pathological staging (pTNM) is the completion of clinical (cTNM) and surgical (sTNM)
staging. The exeresis material varies with the type of surgery (lung, lobe,
segments, tumorectomy). The pTNM reflects the removed material, so there is a
need for the lymph node stations to be removed during surgery to evaluate the N
parameter:
N1 ilari lymph nodes (around the main bronchus), interlobars (around lobar
bronchi) and intraparenchymal (lobar, segmental and subsegmental) - are found by
the pathologist.
N2 - homolateral mediastinal lymph nodes -,
N3 - contralateral mediastinal lymph nodes are found and identified by the
surgeon.
Parameter M is evaluated when material is taken from a suspected metastasis. The
possible negativity does not naturally allow to exclude metastases in other
locations, for which the abbreviation Mx is used, rather than M0.
Treatment
The therapy is configured in three types of intervention:
surgery
radiotherapy intervention
chemotherapeutic intervention
radiofrequency ablation or thermal ablation
mixed interventions
monoclonal therapy
It must be entrusted to expert hands, in centers of consolidated experience and
that apply the most appropriate therapeutic protocols.
To learn more >>
Lung cancer, why
Classification of lung tumorsi
The solitary nodule of the lung
Noduli polmonari: diagnosi
di natura
index tumor
 Meanwhile, the first thing to do is to know what to look for, because the doctor
does not always know it! In fact, before making a diagnosis, it is necessary to
have carried out the proper investigations and to have carried out the
instrumental assessments of the case. If a patient always has cough or chronic
bronchitis, a neoplastic lesion should be suspected that underlies the pathology
I am treating.
Meanwhile, the first thing to do is to know what to look for, because the doctor
does not always know it! In fact, before making a diagnosis, it is necessary to
have carried out the proper investigations and to have carried out the
instrumental assessments of the case. If a patient always has cough or chronic
bronchitis, a neoplastic lesion should be suspected that underlies the pathology
I am treating. Often the signs are strange: a patient had lost weight and could no longer feed
as he should. Initially aside from an insistent cough, the patient loses weight
and does not feed, has disgust for the foods he previously thought to be appetizing,
presents dyspnea, chest pain, blood-stained or frankly blood-stained sputum,
bone pain especially if metastases are present , clubbing, serotine fevers,
fever that heals by antibiotic treatment but then resumes,
asthenia. Other times it shows signs of
relevance of the mediastinal syndrome.
Often the signs are strange: a patient had lost weight and could no longer feed
as he should. Initially aside from an insistent cough, the patient loses weight
and does not feed, has disgust for the foods he previously thought to be appetizing,
presents dyspnea, chest pain, blood-stained or frankly blood-stained sputum,
bone pain especially if metastases are present , clubbing, serotine fevers,
fever that heals by antibiotic treatment but then resumes,
asthenia. Other times it shows signs of
relevance of the mediastinal syndrome. • Currently lung cancer is the most frequent malignant neoplasm and the main
(17% of all cases) cause death from neoplasm in the world both in males (24% of
all cases) and in females (10% of all cases ) with over 3,000 deaths a day
worldwide.
• Currently lung cancer is the most frequent malignant neoplasm and the main
(17% of all cases) cause death from neoplasm in the world both in males (24% of
all cases) and in females (10% of all cases ) with over 3,000 deaths a day
worldwide.