 Clearly the information contained here is a reading: no one can replace your
doctor, because caring for the heart is a dangerous and delicate topic.
Clearly the information contained here is a reading: no one can replace your
doctor, because caring for the heart is a dangerous and delicate topic.
If the
drugs are dosed little or bad, you run the risk of serious complications. A
practical tip is to always check your blood pressure and, above all, to measure
the electrolytes, sodium and potassium, and to control regularly kidney function.
Diuretics should not be used alone (even if the symptoms of SC are controlled),
but should be used in combination with other drugs, such as, if not
contraindicated and tolerated, ACE-I, digoxin and beta-blockers (Consensus
Recommendations for the Management of Chronic Heart Failure, 1999) and the good
and dear anti-aldosterones, e.g. the canrenoato or luvion. If you read this page,
it means that your cardiologist does not follow you as it should. In fact, you
find your legs swollen, you miss the air, you can not wear the old elegant shoes
and when you lie down you need the pillows. The night then is a pain: you get up
with trouble to urinate. Let's see how to implement good care. Diuretics, in
fact, induce a possible further activation of the angiotensinine
renin-aldosterone system (RAA), which can mitigate its effectiveness. For this
reason they are not recommended in monotherapy and should be used together with
drugs that can counterbalance the negative effects of neuro-hormonal stimulation.
In the initial therapy the following general indications can be adopted, with
some precautions:
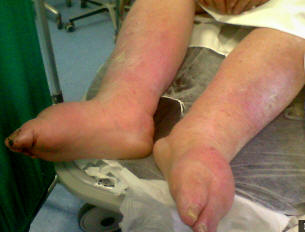 Imposing declining edemas (note the swollen feet) in elderly patient with heart failure in NYHA class 3-4 |
• Loop diuretics: for their effects they are the
preferred agents in SC therapy; furosemide, torasemide, piretanide and
bumetanide are the most frequently used in the treatment of patients with
heart failure.
In chronic SC, the initial posology of furosemide is 25-50 mg / day per os, with
increased dosage up to an increase in effective diuresis to reduce weight by at
least 0.5-1 kg / day. Since the half-life of loop diuretics (except torasemide)
is short (1.5-2 hours for furosemide, 1 hour for bumetanide) (short-acting
diuretics), often more daily doses are required: if not coexisting renal
insufficiency should be administered at least three times a day. The problem is
that in the most serious cases, the furosemide dosage is increased: generally
the patient takes 1/4 cpr of 500 mg / bid furosemide. In this case the risk of
severe hyponatraemia is very easy. The patient appears in a coma, as if he had a
stroke, with values of natality of 105 mmol / L. This occurrence is very
frequent in the hospital.Torasemide, which has a greater intrinsic diuretic potential (about double-triple), a higher
bioavailability (over 80% per os) and a longer half-life than furosemide, seems
able, according to randomized studies, to reduce hospitalizations,
cardio-vascular events (Noe et al.) and costs (Stroupe et al.) in SC.
The efficacy of torasemide is associated with a safe use, particularly on the metabolic and electrolytic profile (Argenziano et al.). The torase-mide is considered by the ACC / AHA 2001 Practice Guidelines among the "commonly used" drugs in the treatment of chronic cardiac scom-think. Some patients with renal failure respond better to torasemide than furosemide for better absorption (Risler et al, 1994). From a prospective study, there would be a lower risk of worsening of SC in patients treated with torasemide compared to furosemide (Murray et al, 1999), but the question remains controversial (ACC / AHA, 2001). Instead, ethacrynic acid should be reserved for patients who do not tolerate sulphonamide derivatives.
• Thiazide diuretics: they are usually useful as a single diuretic drug
in the treatment of water retention only in patients with mild heart failure,
since their site of action at the level of the distal nephron allows for the
rapid adjustment of the intrarenal absorption of water and solutes at the level
of the other more proximal segments of the nephron. Thiazide diuretics are less
effective in patients with moderate renal impairment (glomerular filtration rate
less than 30 ml / minute) and in these cases thiazides should not be used,
except in combination with loop diuretics, with which they present a true
synergism, determining a natriuresis greater than the sum of that given by each
class of drugs. This property is useful in treating resistance to diuretics. The
metolazone is a benzothiazide diuretic (thiazido-like) diuretic burdened by
conspicuous side effects (such as a marked depletion of electrolytes and
metabolic alkalosis) that should be reserved for cases of refractory
decompensation one-two times a week, with senate control of serum electrolytes.
• Potassium-sparing diuretics: they are not effective when used alone in
the treatment of heart failure. However, they are useful in limiting the loss of
potassium and magnesium in association with loop diuretics. Potassium-sparing
diuretics should be administered with caution to patients receiving drugs that
antagonize the renin-angiotensin-aldostero-ne system (RAAS) such as ACE
inhibitors, which increase potassium plasmática concentration. Beta-adrenergic
antagonists and non-steroidal anti-inflammatory drugs (NSAIDs) may also induce
hyperkalaemia in patients receiving potassium-sparing diuretics. The use of
potassium-sparing diuretics (triamterene, amiloride, spironolactone) is useful
in combination with thiazides to prevent hypokalemia (oral potassium supplements
are usually ineffective). It is advisable to start with low doses in the first
week. The association with ACE-I requires close control of potassium.
RESISTANCE TO DIURETICS: DEFINITION AND CAUSES
Individually administered loop diuretics are generally effective in advanced
congestive heart failure and the highest acute natriuretic response is achieved
in a short time. However, as in the absence of heart failure, some compensatory
mechanisms may limit the diuretic response of the patient to the next dose of
diuretic. These variations are the result of alterations of the intrarenal
hemodynamics induced by the diuretics themselves [: me result of a
tubulo-glomerular feedback and an increased activity of the sympathetic nervous
system (adaptation to diuretics). It is defined resistance to diuretics in the
patient with congestive-edematous SC the clinical condition in which the
diuretic response is reduced or lost before the therapeutic objective (reduction-resolution
- edema) is reached.
The chronic use of diuretics stimulates the renin-angiotensin-aldosterone system
(RAAS), with morpho-functional modifications of the nephron and
counterproductive neurormonal adaptive responses, such as the increase in
plasmase activity and sympathetic stimulation, which increases the afterload ,
can lead to a worse prognosis of patients (David, 2001).
The risks of the diuretic treatment of SC are schematically linked to the
following (Consensus Recommendations for the Mana- gement of Chronic Heart
Failure, 1999).
• Hypovolemia and hypotension: in any case, postural changes of blood pressure,
smoothing of the jugular veins and rapid and progressive worsening of renal
function must be suspected. The presence of an arterial hypotension should be
systematically sought during diuretic therapy in heart failure, particularly in
the elderly and in patients with SC from diastolic dysfunction (often elderly);
in these patients it is therefore necessary to check specifically:
- the existence of orthostatic hypotension;
- the existence of post-prandial hypotension.
- Orthostatic hypotension generally responds to the reduction / suspension, if
possible, of diuretic therapy or vasodilators.
The hypovolaemia associated with hypotension <80 mmHg can, at times, require the
careful infusion and with close patient haemodynamic monitoring of 500-1000 ml
saline solution, with the aim of tracing the PAS up to 100 mmHg in a short time
.
• Hyperazotemia and renal insufficiency, secondary to hypovolaemia, can further
worsen, together with hypotension, SC; diuretic-induced hyperazotemia is
generally moderate and reversible after drug withdrawal, but in some cases
intensive diuretic therapy involving weight loss> to 2 kg may, particularly in
patients with impaired renal function, result in severe deterioration of renal
function with increased mortality (Weinfeld et al.).
• Depletion of electrolytes (potassium and magnesium): it is related to the
increased distribution of sodium in the distal tubules and to the exchange of
sodium with other cations; this process is enhanced by the activation of the RAA
system, a frequent phenomenon in heart failure. Electrolyte depletion is greater
in case of loop diuretic association with thiazides. Hypokalemia may be treated
with concomitant use of drugs that inhibit the release of aldosterone (ACE-I) or
prevent the receptor binding (spironolactone and other antialdosterones) or
reduce the loss of potassium in the distal nephron (amiloride) .
Recommendation
- Diuretic therapy patients should undergo a control of blood potassium
frequently, in particular:
- at the beginning of the therapy;
- during the titration;
- contextually to any variation of diuretic therapy.
Potassiemia is an inaccurate indicator of total body potassium reserves (patients
with normal potassium may have reduced levels of body potassium); in patients at
high risk it may also be useful to evaluate urinary excretion in the 24 hours of
potassium.
• All patients with a blood pressure <3.5 mEq / 1 should receive potassium
sparing diuretics if already treated with ACE-I.
• Although the efficacy of oral potassium supplements has been questioned (European
Society of Cardiology, 1997), it is recommended that they be administered in
amounts of 20 and 40-100 mEq / day respectively for its prevention or its
treatment (Cohn et al.).
• Potassium depletion is frequently accompanied by magnesium depletion, which
must be controlled at the same time, especially if high doses of diuretics are
used.
• Neurohormonal activation: particularly of the renin-angio-tensin-aldosterone
system, with negative consequences on the further progression of heart failure
and possible refractoriness to diuretics; this effect seems more pronounced for
"short-acting" diuretics (furo-semide) than those with a more prolonged action (Tomiyama).
• Metabolic alkalosis: usually related to hypochloraemia, may also depend on an
increased Na + / H + exchange and increased sodium availability in the
collecting tubule and increased aldosterone secretion in the distal tubule. More
often than moderate, it can sometimes be severe; manifests itself with some
diuretics, such as those of the loop or the metolazone.
• Other metabolic effects: hyperglycaemia, resistance and reduced insulin
secretion, non-keto-acidotic hyperosmolar states.
• Deficiency of water-soluble vitamins: thiamine and ascorbic acid deficiency
can exacerbate the refractory edema in heart failure, making it the most
problematic therapeutic management (Constant).