The circulatory system, heart and arteries
- Gastroepato
- Cardiology
- The circulatory system, Heart
and arteries
- Cardiovascular risk and
its factors
- The patient swollen
- Practical anatomy of
the heart and large
vessels

 notes by dr Claudio Italiano
notes by dr Claudio Italiano
To live and work, tissues and organs need nourishment and energy. Therefore the
glucose and the oxygen necessary for the chemical "combustion" of the same
glucose must come into the whole body, which occurs, as we know, at 37 ° C, with
a remarkable energy yield.
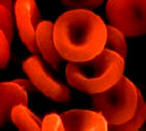 The main functions of the circulatory system, therefore, consist in the
circulation of the blood tissue throughout the body, which is in turn made up,
on one side corpus colata, the red blood cells, and a liquid, the plasma.
The main functions of the circulatory system, therefore, consist in the
circulation of the blood tissue throughout the body, which is in turn made up,
on one side corpus colata, the red blood cells, and a liquid, the plasma.
In the blood where, as we said, we find the red blood cells, they contain within
them a protein called "hemoglobin", consisting of a prosthetic group, the heme
and the globin; the iron contained in the heme has the task of oxidizing, that
is, of picking up oxygen and transferring it to the tissues, a function that
normally occurs when the organism is in physiological conditions.
However, there are conditions in which the respiratory function and the exchange
of oxygen, emitted, does not occur through carbon monoxide poisoning. At other
times, the bloodstream, due to conditions of myocardial decompensation, does not
take place adequately with respect to the organism's needs, so that a person who
lives in a state of decompensation is barely able to move a few steps and
presents worsening dyspnea even to minimal efforts.
To reach all points, we said, blood must circulate through the blood vessels
to the human body, and this is possible thanks to a pump, the heart, the
delivery vessels, the arteries, the vessels specialized for the venous return to
the heart that is, the veins, and the capillaries, which are the small vessels
used for the exchange in the tissues.
 It is the body responsible for circulation as a pump. It has an almost conical
shape that has an elongated upper base and a "tip" (apex) facing slightly to the
left. The base is inclined towards the vertebrae and as well as the left side.
The heart is made up of three tonics from the inside to the outside: endocardium
(with the same functions and same structure as the endothelium), myocardium (hybrid
muscle between smooth and striated: it has the ability to contract rhythmically,
but involuntarily.
It is the body responsible for circulation as a pump. It has an almost conical
shape that has an elongated upper base and a "tip" (apex) facing slightly to the
left. The base is inclined towards the vertebrae and as well as the left side.
The heart is made up of three tonics from the inside to the outside: endocardium
(with the same functions and same structure as the endothelium), myocardium (hybrid
muscle between smooth and striated: it has the ability to contract rhythmically,
but involuntarily.
It is made up of cells with semi-organized contractile proteins - more organized
than smooth muscles, but less than striated muscles. The cells are 100-500
microns long and have a diameter of 100-200 microns). Finally, in the outermost
layer is the epicardium (equal to the adventitia habit of the vessels). In
addition to the vessels, however, the heart also has an additional coating: a
fibrous sac called fibrous pericardium and a second sac called a parietal
leaflet.
Between the latter and the epicardium (which together form the serous
pericardium) a fluid (fluid of the pericardial cavity) is interposed that allows
the heart to move freely in the sac. The circulation of the heart is ensured by
the coronary system, which originates from the aorta artery as a small artery
that forks into two branches, the right coronary artery and the left coronary
artery. The course on the right hand side marks the border between the right
atrium and the right ventricle.
This artery sends two branches down, the right marginal branch and the anterior
cardiac artery. The left coronary artery divides into a circumflex artery, whose
course marks the division between left atrium and left ventricle, and anterior
interventricular artery, which marks the border between left ventricle and right
ventricle. In addition to these it also produces other small arterial twigs.
The circumflex artery and right coronary artery turn behind the heart and join.
The second sends a branch (posterior interventricular artery) that marks the
limit between left ventricle and right ventricle. Further on sends another
branch, the posterior branch of the right coronary artery.
As the circumflex artery, send a branch called the left marginal branch of the
left coronary artery. The inferior vena cava and the superior vena respectively
flow into the lower and upper part of the right atrium. From the right ventricle
the small circulation starts, that is the flow of blood directed to the lungs,
through the pulmonary artery.
After exchanging carbon dioxide for oxygen to the lung, the blood returns to
the heart via 4 pulmonary veins (two from the right lung and 2 from the left) of
0.5 cm of diameter, in the left atrium.

 Classically, if we dissect the heart in a frontal way, 4 cavities appear, two on
the left and two on the right, subdivided by a septum.
Classically, if we dissect the heart in a frontal way, 4 cavities appear, two on
the left and two on the right, subdivided by a septum.
The right atrium has thin walls and as it was said it receives the blood from
the inferior vena cava and the superior vena cava.
The blood falls due to pressure difference towards the underlying chamber (right
ventricle), after which the atrial systole intervenes and sends it into the
ventricle through the tricuspid valve.
In the right atrium (near the orifice of the inferior vena cava) there is also a
scar, due to the closure of the Botallo hole, which makes the atria communicate,
during the intrauterine life. The right ventricle rests on the front face of the
diaphragm.
It receives blood from the right atrium and sends it, with the ventricular
systole, to the pulmonary artery, so that it is carried to the lungs to
oxygenate and discard carbon dioxide. The closure of the tricuspid valve (beginning
of the systole) constitutes the first cardiac tone ("tum"), a dark and long
sound (see auscultation of the heart).
The closing of the pulmonary semilunar valve (between the ventricle and the
pulmonary artery, which has three semilunar cusps: right, left and anterior) is
the second cardiac tone ("ta"), is shorter, dry and clear and also marks the end
of systole ventricular.
Ventricular systole is powerful and blood pressure is quite high (about 40 mmHg);
enough to break through the tricuspid (because it acts on the opposite side).
But the valve does not break because three muscular papillae are erected from
the wall of the ventricle, which are the point of attack of three
ultra-resistant fibrous bundles (tendon ropes) that support the tricuspid and
help it to open and, above all, to close and to remain closed. The lung
semilunar opens for blood pressure, so it does not need ropes to hold it.
The part of the ventricle in which the pulmonary semilunar is positioned is
called infundibulum. If the valves do not work well, they produce a different
tone, which can be perceived with the phonendoscope. The upper left cavity is
called the left atrium. It is a cavity with rather thin walls.
Receives oxygenated blood from the lungs and sends it into the left ventricle;
blood falls by gravity, but then the atrial systole squeezes the atrium and
empties it completely. In the left atrium, 4 veins (the pulmonary veins, 2 per
lung) are inserted, which carry the oxygenated blood from the lungs (therefore
arterial) to the heart; these are called veins even if they carry arterial blood,
because, by convention, every vessel that carries blood to the heart is called a
vein. The left ventricle is the largest and most powerful cavity in the heart.
It is located in the lower left portion and is very close to the left lung, from
which it is separated only by the pericardium and the pleura.
It receives the oxygenated blood from the left atrium, through the bicuspid or
mitral valve, and sends it, through the systole (7 times more powerful than the
right ventricle), into the aorta, since it reaches the whole body, including
myocardium.
Between the ventricle and the aorta a semi-lunar valve is interposed: the aortic
semilunar valve (which has three semilunar cusps: right, left and posterior).
The contraction of the ventricle is very powerful so the mitral must be kept in
place, otherwise it would be broken down.
For this purpose there are two fibrous bundles, larger than those of the right
ventricle, supported by two large muscular papillae, larger than those of the
right ventricle, which rise from the wall of the heart.
Also in this part of the heart there are two heart tones: the first ("tum") is
the closing of the mitral valve, the second ("ta") is the closure of the aortic
valve. Also on this side, if the valves do not work well, they produce a
different tone, which can be perceived with phonendoscope.
 The arteries, that is the delivery vessels, start from the heart starting with
the main artery, ie the aorta, which directly from the left ventricle of the
heart, where it presents to its origin a valve that has the task of allowing the
flow only towards a direction, receives oxygen-rich blood and distributes it to
the brain, arms, and whole body.
The arteries, that is the delivery vessels, start from the heart starting with
the main artery, ie the aorta, which directly from the left ventricle of the
heart, where it presents to its origin a valve that has the task of allowing the
flow only towards a direction, receives oxygen-rich blood and distributes it to
the brain, arms, and whole body.
In fact, the aorta is presented in its first portion of arched shape, and
immediately leads up and to the right as the ascending aorta, forming the arch
of the aorta, a sort of vase in the shape of an "umbrella handle" , from which
the left subclavian branch, the left common carotid and the common
brachycephalic trunk or anonymous artery branch off.
The arch continues with the abdominal aorta.
From the sinuses of left and right Valsalva originate the two coronary arteries,
right and left, which supply the arterial blood to the heart. In addition,
Valsava aortic sinuses that contain receptors for the quality of the blood are
present. The aortic arch goes up and to the left and then curves down and to the
left.
It is in relationship with the pulmonary trunk inferiorly and anteriorly, with
the right pulmonary artery inferiorly and posteriorly, with the left pulmonary
artery inferiorly and anteriorly, with the trachea and the bronchi superior and
posteriorly, with the lungs laterally, with the vena cava superior, its
brachiocephalic trunks and the body of the sternum anteriorly, with the
insertions of the sternioid and thyroid muscles superiorly, with the phrenic
nerves and left vagus to the left and with the esophagus which in this tract is
the latter.
The aorta continues as a descending aorta which is divided into two sections,
thoracic and abdominal, divided by the diaphragm. The thoracic aorta thus leads
behind the esophagus, remaining in posterior contact with the thoracic duct and
vertebral bodies and penetrating into the abdomen through the aortic hiatus of
the diaphragm.
Along its course it gives parietal branches (posterior intercostal arteries,
musculocutaneous arteries and vertebromidullary arteries) and visceral branches
(esophageal arteries, bronchial and tracheal arteries and posterior mediastinal
arteries). All the ascending aorta, the aortic arch and the thoracic portion of
the descending aorta are found in the mediastinum, the cavity that contains the
heart.
The abdominal aorta is instead retro-peritoneal, in the abdomen. It is carried
in the abdomen through the medial pillars of the diaphragm under the median
arched ligament (aortic hiatus) and from this position it is posterior to the
stomach, liver, pancreas, duodenum, intestines and their meso. It maintains
contact with the bodies of the vertebrae.
In the abdomen the aorta gives numerous branches, parietal and visceral. In the
cephalocaudal order are the lower frenetic arteries, for the inferior face of
the diaphragm, the lumbar arteries, distributed along the whole abdominal aorta
and which vascularize the walls of the abdomen with the last intercostal
arteries, the celiac trunk, unequal branch deputizing to the vasculature of the
spleen, abdominal part of the esophagus, stomach, liver, upper part of the
pancreas and duodenum, upper mesenteric artery (see arteriography of the celiac
tripod), unequal branch responsible for spraying the pancreas and duodenum, the
totality of fasting and ileum, of the whole ascending colon and of the right
half of the transverse colon, the average adrenal arteries, which vascularize
part of the adrenal anastomoses with the upper adrenal arteries, branches of the
lower frictures and with the inferior adrenal arteries, branches of the renal
arteries, arteries kidneys, which vascularize the kidneys and their capsule, the
genital or gonadal arteries, sperm in the male and ovaries n the females, which
vascularize the testes or ovaries and the inferior mesenteric artery, unequal
branch deputized to vascularize the left half of the transverse colon, the
entire descending colon, the whole sigma and the upper part of the rectum (with
the rectal artery or upper hemorrhoidal).
The abdominal descending aorta ends at the level of the fourth lumbar vertebra
dividing into its three terminal branches. The median branch, the median sacral
artery is a thin branch destined to the vascularization of the sacrum and the
piriformis muscle, and yields an even branch, the lumbar artery ima for the
parietal vascularization of the lower abdomen. The two lateral branches, much
larger than the previous one, are the two common iliac arteries, responsible for
the vascularization of the pelvis, the gluteal region and the entire lower limb.
index cardiology
 notes by dr Claudio Italiano
notes by dr Claudio Italiano
 notes by dr Claudio Italiano
notes by dr Claudio Italiano
 The main functions of the circulatory system, therefore, consist in the
circulation of the blood tissue throughout the body, which is in turn made up,
on one side corpus colata, the red blood cells, and a liquid, the plasma.
The main functions of the circulatory system, therefore, consist in the
circulation of the blood tissue throughout the body, which is in turn made up,
on one side corpus colata, the red blood cells, and a liquid, the plasma. It is the body responsible for circulation as a pump. It has an almost conical
shape that has an elongated upper base and a "tip" (apex) facing slightly to the
left. The base is inclined towards the vertebrae and as well as the left side.
The heart is made up of three tonics from the inside to the outside: endocardium
(with the same functions and same structure as the endothelium), myocardium (hybrid
muscle between smooth and striated: it has the ability to contract rhythmically,
but involuntarily.
It is the body responsible for circulation as a pump. It has an almost conical
shape that has an elongated upper base and a "tip" (apex) facing slightly to the
left. The base is inclined towards the vertebrae and as well as the left side.
The heart is made up of three tonics from the inside to the outside: endocardium
(with the same functions and same structure as the endothelium), myocardium (hybrid
muscle between smooth and striated: it has the ability to contract rhythmically,
but involuntarily.
 Classically, if we dissect the heart in a frontal way, 4 cavities appear, two on
the left and two on the right, subdivided by a septum.
Classically, if we dissect the heart in a frontal way, 4 cavities appear, two on
the left and two on the right, subdivided by a septum.
 The arteries, that is the delivery vessels, start from the heart starting with
the main artery, ie the aorta, which directly from the left ventricle of the
heart, where it presents to its origin a valve that has the task of allowing the
flow only towards a direction, receives oxygen-rich blood and distributes it to
the brain, arms, and whole body.
The arteries, that is the delivery vessels, start from the heart starting with
the main artery, ie the aorta, which directly from the left ventricle of the
heart, where it presents to its origin a valve that has the task of allowing the
flow only towards a direction, receives oxygen-rich blood and distributes it to
the brain, arms, and whole body.